What are the expectations of a perfusionist career?
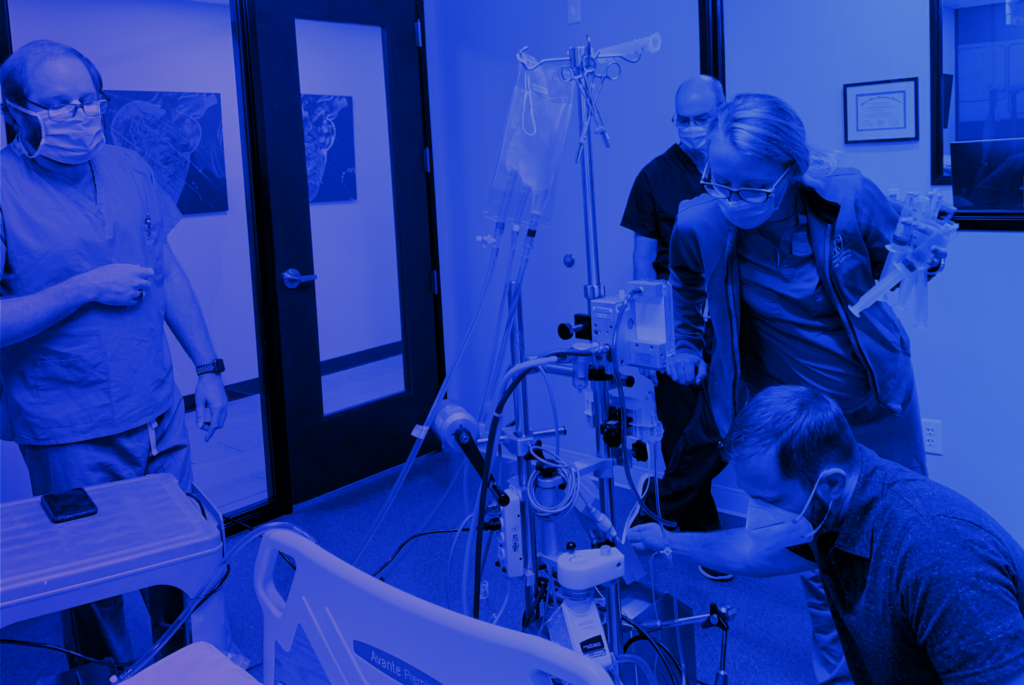
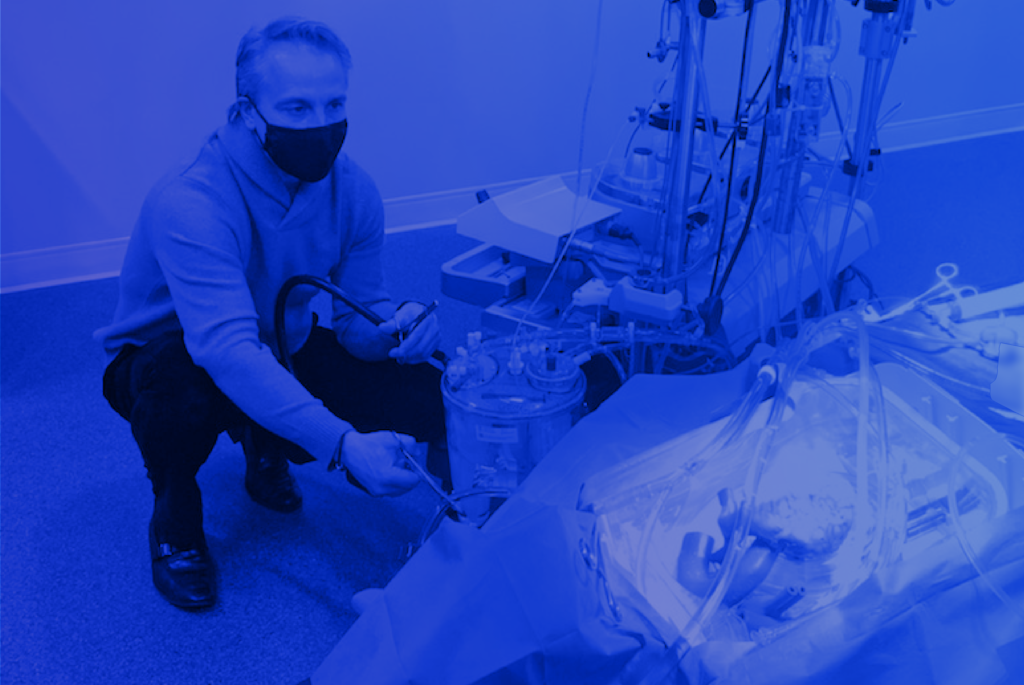
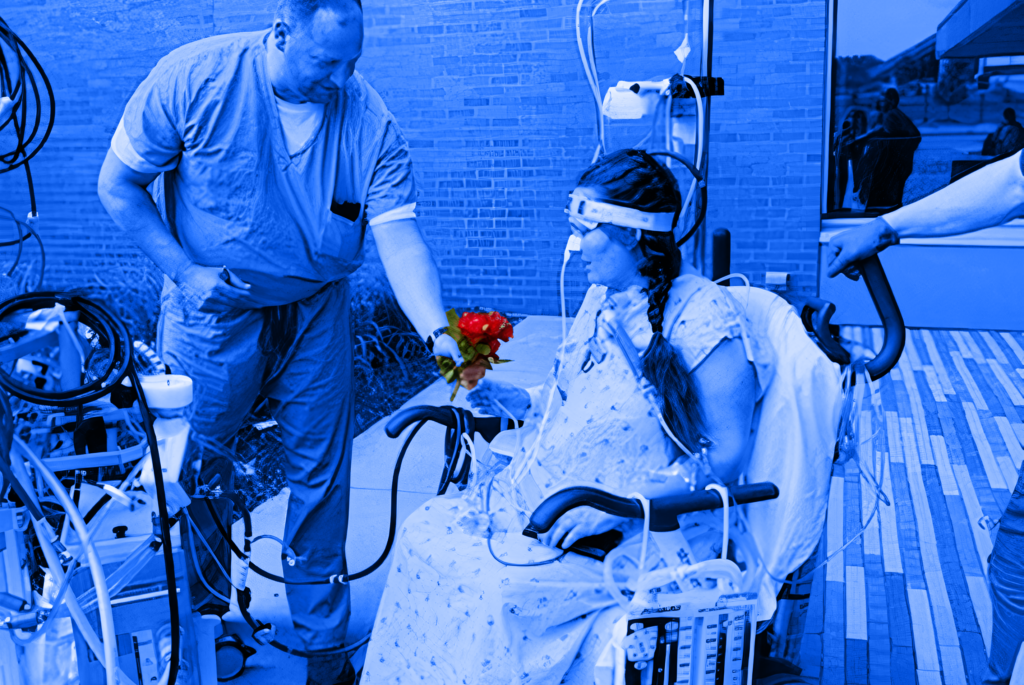
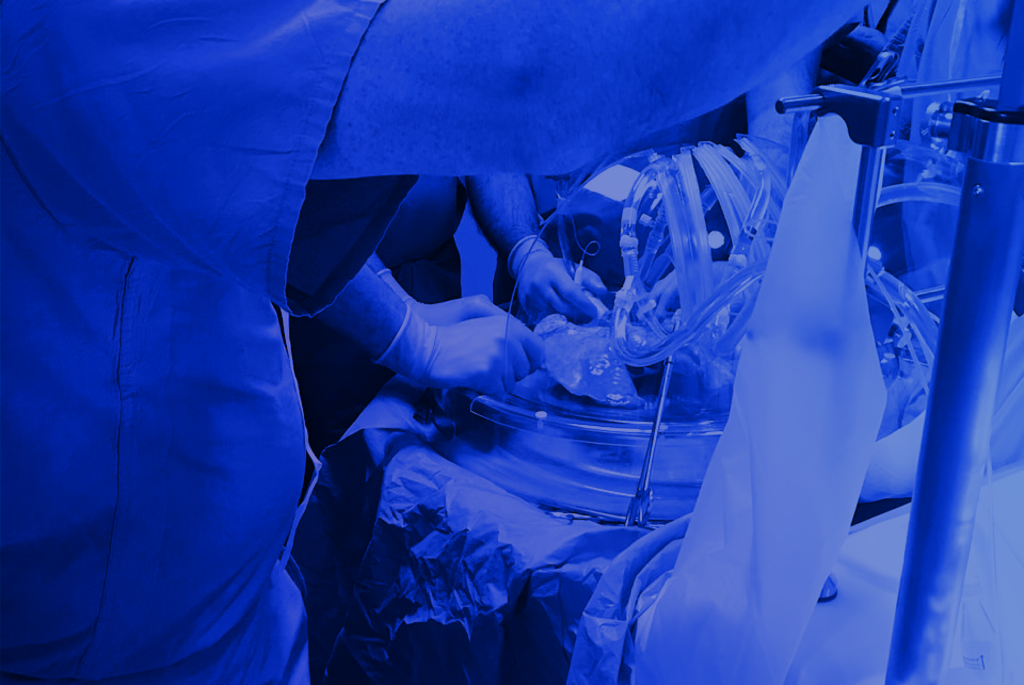
For those with a strong background or interest in healthcare and science, a career working as a perfusionist can be highly rewarding. Perfusionists work as key members of cardiovascular surgical teams by using specialized equipment and patient monitoring techniques. Let’s find out more about this exciting career path essential to the practice of modern medicine. […]
What are the expectations of a perfusionist career? Read More »